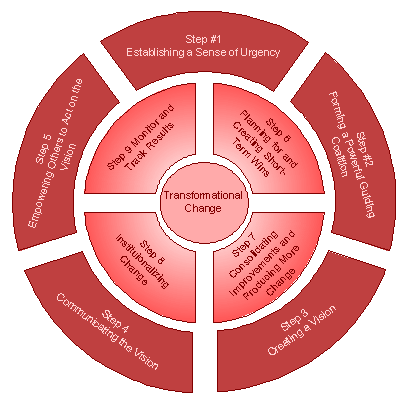
Realization of savings and resulting budget reductions from standardization and utilization initiatives will necessitate significant change management initiatives and an institutionalizing of new approaches that can withstand the rigors of time.
SCA’s approach involves the application of proven methodologies to effect transformational change in supply chain processes. Industry leading, change management methodologies have been adapted and modified to be relevant in today’s healthcare environment specifically with physician cultures.
SCA’s approach involves the application of proven methodologies to effect transformational change in supply chain processes. Industry leading, change management methodologies have been adapted and modified to be relevant in today’s healthcare environment specifically with physician cultures.
Examples of change efforts that will be instrumental to achieving success with clinical supply cost management initiatives include:
Effective Use of Data - Establishing Internal Best Practices
Another critical part of our approach to driving change, particularly with physicians and other clinicians, is effective use of data, which can demonstrate that the desired change does not comprise the quality of care. The most valuable data to drive change in the use of clinical supply expenses are micro-level departmental or procedural metrics that are specific to the organization and measure performance over time against defined goals. At this level, performance improvements are driven through the identification and reduction of procedural and resource utilization variation within the system. These benchmarks/metrics provide a foundation to evaluate and compare practice patterns among physicians and across hospitals down to specific drugs, supplies, lab tests, imaging procedures, etc.
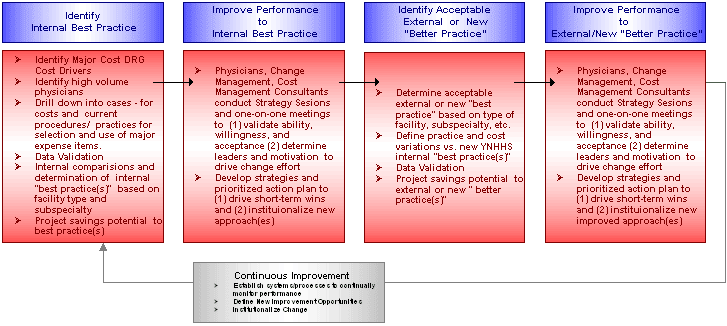
Synergy Consulting Associates’ approach to physician preference items is designed to foster physician and clinician acceptance and the achievement of lower procedural costs by first defining and aligning to internal “best practice,” and then moving to identification and alignment to a potentially “better” external or new practice. We believe this approach best addresses the complex and unique environment of each individual healthcare system.
- create a vision that is meaningful to physicians and clinicians
- change to the systems and structures that under gird the vision (e.g., create strategic vendor partnerships that are based on standardization and utilization goals rather than just price)
- establish incentives that reinvest portions of savings into new technologies
- minimize variability and waste in processes
Effective Use of Data - Establishing Internal Best Practices
Another critical part of our approach to driving change, particularly with physicians and other clinicians, is effective use of data, which can demonstrate that the desired change does not comprise the quality of care. The most valuable data to drive change in the use of clinical supply expenses are micro-level departmental or procedural metrics that are specific to the organization and measure performance over time against defined goals. At this level, performance improvements are driven through the identification and reduction of procedural and resource utilization variation within the system. These benchmarks/metrics provide a foundation to evaluate and compare practice patterns among physicians and across hospitals down to specific drugs, supplies, lab tests, imaging procedures, etc.
Synergy Consulting Associates’ approach to physician preference items is designed to foster physician and clinician acceptance and the achievement of lower procedural costs by first defining and aligning to internal “best practice,” and then moving to identification and alignment to a potentially “better” external or new practice. We believe this approach best addresses the complex and unique environment of each individual healthcare system.
This approach also eliminates the first hurdle and physician objection normally confronted with the use of external benchmarks “we’re different” and the selected comparative universe isn’t comparable. Although objectivity and size of external benchmarks can be valuable in defining “better” standards of performance, the perceived relevance can establish obstacles that hinder progress towards change. Starting with internal “best practices” and definition of what realistic cost structures should be based on uniqueness of the system, including reimbursement, provides the physician with “acceptable” data to change behavior and see measurement as a means for improvement and not judgment.